Feed the Baby
When the Baby Needs Extra Help
By Beverly Morgan, IBCLC, Kim Evangelisti & Caroline L. Bias, M.S., CCC-SLP

Lactation consultants say that the first rule is to “feed the baby” in a way that is comfortable as well as efficient for weight gain and development. Even though in some cases the most efficient feeding method may not be the traditional method of getting milk from the breast, there are many options available for supplementing with breast milk or formula. Babies that need supplemental feeding may need it short term—— a feeding or two— or long term. Alternative feeding methods are tailored to fit the unique needs of each mother/infant pair. Some mothers may need to use the alternative methods for the entire feedings and others may need the alternative methods for just part of some feedings. In our descriptions here we are not making an assumption that the baby is fed exclusively with any of the methods. Indeed, one baby may experience several feeding methods before going on to breastfeed.
This article will briefly introduce a variety of feeding devices. Some you may know about, others you may not have seen or considered. These feeding methods can help a baby with feeding challenges get the food he needs to thrive.
(NB: Picture used with permission)
This article will briefly introduce a variety of feeding devices. Some you may know about, others you may not have seen or considered. These feeding methods can help a baby with feeding challenges get the food he needs to thrive.
(NB: Picture used with permission)
Breastmilk or Formula?
If a baby needs to use a feeding method other than direct breastfeeding his mother will need to use a breast pump in order to protect her milk supply.
Generally the earlier the mother recognizes the baby’s need to have additional feedings, the better her chance to protect her milk supply. In some cases it is clear where the problems originated. At other times it can be difficult at first, to discern if the difficulty comes from the mother’s reduced milk supply, or the baby’s inability to get the milk he needs at the breasts.
Mothers own milk is the food of choice. Milk from a milk bank is also a possibility for a baby when receiving his own mother’s milk is not. Formula is usually the choice of last resort for mothers committed to giving their babies their breastmilk, but it is important to remember to “feed the baby” and sometimes formula is the only possible option. In the early days especially, the volume of milk the baby needs is small. The benefits of human milk for little humans is well documented. Pumps and banked milk may well be covered medical expenses. When human milk is not available health care professionals will help parents choose from the formulas available to them.
Generally the earlier the mother recognizes the baby’s need to have additional feedings, the better her chance to protect her milk supply. In some cases it is clear where the problems originated. At other times it can be difficult at first, to discern if the difficulty comes from the mother’s reduced milk supply, or the baby’s inability to get the milk he needs at the breasts.
Mothers own milk is the food of choice. Milk from a milk bank is also a possibility for a baby when receiving his own mother’s milk is not. Formula is usually the choice of last resort for mothers committed to giving their babies their breastmilk, but it is important to remember to “feed the baby” and sometimes formula is the only possible option. In the early days especially, the volume of milk the baby needs is small. The benefits of human milk for little humans is well documented. Pumps and banked milk may well be covered medical expenses. When human milk is not available health care professionals will help parents choose from the formulas available to them.
Babies who often Need Extra Help with Breastfeeding
In many cases a baby needs to increase her strength or skills to be able to nurse. In other situations the baby may need corrective surgery, for example, a tight fermium clipped or a cleft repaired. He may need therapy such as oral motor therapy for oral aversion or physical therapy for a tight, stiff neck which interferes with breastfeeding. The following is a list of some of the situations that frequently require extra help with feeding.
If your baby is not gaining weight effectively or if he shows unhappiness or frustration with feeding, ask your health care provider, IBCLC, or feeding therapist about feeding methods that might be helpful for your baby.
- Premature babies
- Near-term babies
- Babies with cleft palate (and possibly cleft lip)
- Babies with oral motor problems
- Babies with Developmental Delays and Disabilities
- Babies who refuse to breastfeed
- Babies who are Hypotonic or hypertonic
- Babies who’s mothers have a partial milk supply
If your baby is not gaining weight effectively or if he shows unhappiness or frustration with feeding, ask your health care provider, IBCLC, or feeding therapist about feeding methods that might be helpful for your baby.
Alternative Feeding Techniques
|
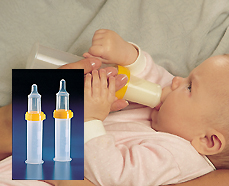
Syringe Feeding Can be Done at Breasts or with a Finger
This is a good method to be sure a baby is getting food in the early days if it is clear the baby will need help getting his nutrition or if the baby is showing distress at the breast. The volume of colostrum is small and feeding the baby by syringe at the breast can assure he is getting enough. He feels successful at the breast as the underlying difficulties are being identified and fixed without the pressure to continue with a poor position or latch. It is often a short term tool, but can be used long term. It is the tool of choice for The Lactation Institute for babies who are not yet able to breastfeed exclusively. |
|
Feeding Devices that Allow Supplementation at the Breast
The Lact-Aid® and the Supplemental Feeding System™ (SNS) ™ by Medela are commercially available feeding aids commonly available in the US. They consist of containers to bring milk to the breast by means of thin tubing. The milk flows from a bottle or bag. In general, using the tool that best fits the baby’s needs will keep him feeling most successful. The SNS™ works well for a child who has an effective suck but needs more milk to flow from the breast. A Lact-aid® works with gravity so it works better for a baby with difficulties removing the milk from the breasts. It does not depend so much on good suction and breastfeeding skills. These devices both work well with expressed breast milk or formula. The Hazelbaker™ Finger Feeder, (FingerFeeder.com), can abe used by placing the tube on the finger or can be used by placing the tube to the breasts. |
|
Spoon Feeding
If baby has to be fed away from the breasts a spoon can be used. In the early days when the baby is receiving a small volume of colostrum or milk. The spoon does not dwarf the volume and allows for slow and steady feeding. One spoon can be placed near the baby’s lips and another spoon used to pour the colostrums or milk into the spoon. A medicine spoon can also be used. |
|
Cup Feeding
Cup feeding can work, even for a newborn. It is a good method for providing milk without introducing artificial nipples. For cup feeding milk is placed in a small, smooth rimmed, shallow cup. The infant can sip the milk from the cup that is placed at his lips. There are specially designed cups for cup feeding an infant or small medicine cups work well too. Medela makes a specialty feeding device called a SoftFeeder™ for use when cup feeding is recommended. It is made from soft silicone and has a special reservoir that controls fluid. Some mothers use this long term when a baby needs milk in another way than direct from the breasts. |
|
Finger Feeding
The finger feeding method involves a tube or syringe that delivers milk to the baby. It can be the tube of a supplemental feeding device or a special one made by Medela called The HazlebakerTM FingerFeeder. In the case of the tube, a small flexible tube is connected to a container of milk--think of it as a small soft drinking straw. It can be taped on a caregiver’s finger. The baby sucks on the finger and receives milk. When using a feeding syringe the baby sucks on the caregiver’s finger and the milk from the syringe is released to run down the finger feeding the baby. These methods work well for incorporating suck retraining and other oral motor therapies. |
|
Nipple Shield
A nipple shield is a thin silicon disk with a nipple that is placed over the mother’s nipple. Nipple shields have been around for a long time. However the ancestors of today’s thin flexible ones were not very effective. The older models did not have much flexibility and didn’t allow for much milk transfer and breast stimulation. The reputation has remained to plague today’s models. Nipple shields can be effective tools. Using nipple shields can result in keeping a baby happy at the breasts who would otherwise become frustrated, overwhelmed, or disinterested in the breast. Many babies need to have a supplemental feeding device in place either over or under the shield to keep the milk flow steady for them depending on why the nipple shield is needed. It is important that he gets the quantity of milk he wants at the flow rate he finds most enjoyable though, or he will quickly reject the shield, and perhaps the breast as well. Other mothers find their babies relax into nursing when they use a nipple shield to moderate mothers too-fast milk flow. Some other babies who do well on nipple shields are ones that are confident with bottle feeding but not breast feeding. A nipple shield may help them become more confident at the breast because the shield feels more like the bottle nipple they are used to. There are other reasons to use a nipple shield. An IBCLC can help you explore if this tool would be helpful for you. |
|
Bottle and Nipple
A bottle is rarely the best first choice. It is best, when possible, for the baby to spend time at the breasts before introducing any other feeding methods. Many of the feeding methods mentioned earlier allow for continued breast feeding even when the baby needs extra help with feeding. Some moms are nervous that use of a bottle will further damage the breastfeeding relationship and prefer other forms of supplementation. Other moms or caregivers find alternate forms of supplementation stressful and prefer to use a bottle, especially when the baby's struggle with breastfeeding continues for weeks or months rather than days. It is not necessarily the bottle and nipple that cause the difficulty. Equally important is the way the baby feels about the method of feeding. If he feels competent with it he is more likely to like it. This highlights how important it is for the baby to feel successful at the breasts and what an important role feeding devices can have in protecting the breastfeeding relationship. Choose a bottle and nipple that seem to help a baby have a relaxed feeding without causing him to get the milk so fast he can hardly breathe or so slow he uses all his energy getting his food. A lactation consultant can help parents find the right balance of breastfeeding and supplementing if needed. Each child and situation is different. |
|
Haberman Feeder
If the baby is refusing to breastfeed and is having difficulties with other feeding methods you may find a specialty feeding nipple like the Haberman Feeder helps to keep him fed. A Haberman Feeder is designed especially for babies with facial or oral problems that interfere with their ability to feed effectively. The nipple has a variable flow rate that is controlled by the person feeding and by the baby based on the baby’s specific needs. It also has a one way valve that prevents flooding the baby with more milk than he can take. This is a commonly suggested feeder for babies with Cleft Palate and those with Velopharyngeal Incompetence because they do not have to achieve suction to be successful. |
|
Feeding Tube
In some cases, a baby is not able to feed safely by mouth, or is not able to get enough by mouth, to achieve nutrition and hydration. In these instances, your physician may recommend a feeding tube for non-oral nutrition. While this news usually comes as quite a shock, it can also be a relief because it takes the pressure off the baby to get enough food. Tube feeding also releases the mother from the near-impossible job of getting a reluctant or ineffective feeder to eat enough to gain weight. Mother and baby can then emphasize bonding in pleasant ways and often can develop feeding skills in a pleasant and relaxed environment. One mother says, “If I knew then what I know now I would not have hesitated to get the g-tube placed much sooner. I really feel like my daughter would be orally eating by now if we had gotten the tube sooner. It made all our lives easier and much happier and allowed us to bond.” When accompanied by effective treatment strategies, the feeding tube can set the stage for a baby to develop oral eating skills without the worry of whether they are consuming enough for nutrition, hydration, and brain development. |
Feeding Tube Options
|
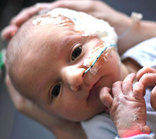
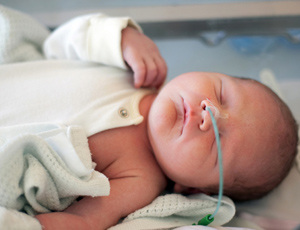
Nasogastric Tubes (NG Tubes)
A nasogastric tube (NG Tube) is a small tube inserted through the nose, down the throat, and into the stomach. While the NG Tube serves the purpose of nourishing a baby, many families see it as a “less invasive, less permanent” interim measure. Since no surgery is necessary to insert an NG Tube families often do a trial run with the NG tube and that trial run can drag on for many weeks or months. When used for extended periods of time, the NG Tube is often associated with increased oral aversion and oral defensiveness. For this reason, many mothers who have “been there” would opt for the surgical tube placement over the NG tube. |
|
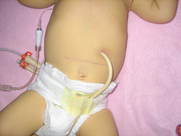
Gastric Tubes (g-tubes), Juojenal Tubes (j-tubes)
Families are often initially reluctant to go with the more “permanent” seeming surgical options such as gastric tubes (g-tubes) inserted into the stomach —or elsewhere in the gastrointestinal tract. If your baby needs a tube for more than a short procedure, the surgical route can often be a BETTER choice because it affords you the opportunity to help them with their oral feeding skills without creating an uncomfortable oral situation. If you are in a situation where your baby requires non-oral nutrition and you have a choice about how it is provided, your doctor can give you additional information about the pros and cons of these options. We also recommend asking to speak to other parents of babies who have had the various types of tube feedings. If your baby is going to require non-oral nutrition of any sort for an extended period of time it is important to get a referral to an oral motor therapist who can help you keep your baby’s mouth and oral areas receptive to eating when they are physically able to do so. Even in infants with severe dysphagia (swallowing disorders) who are aspirating and can’t have anything by mouth, it is critical to effectively stimulate the muscles and sensory pathways associated with eating and eventually speaking in order to prepare the child for later attempts at eating and talking. |
This article has provided you with information about a variety of alternative feeding options for your breastfed infant. Please review the related articles for more information about your specific challenges.